Platelet clinical best practices
Author: Rob Romans, ART, BSc
Online publication date: August 2019
Background
In August 2018, the National Advisory Committee on Blood and Blood Products (NAC) endorsed the document “Guidance on Platelet Transfusion for Patients With Hypoproliferative Thrombocytopenia” published by the International Collaboration for Transfusion Medicine Guidelines (ICTMG).1, 2, 3
To assess current platelet transfusion practice and alignment with these clinical guidelines in Canada, Canadian Blood Services conducted a survey in late spring 2019.
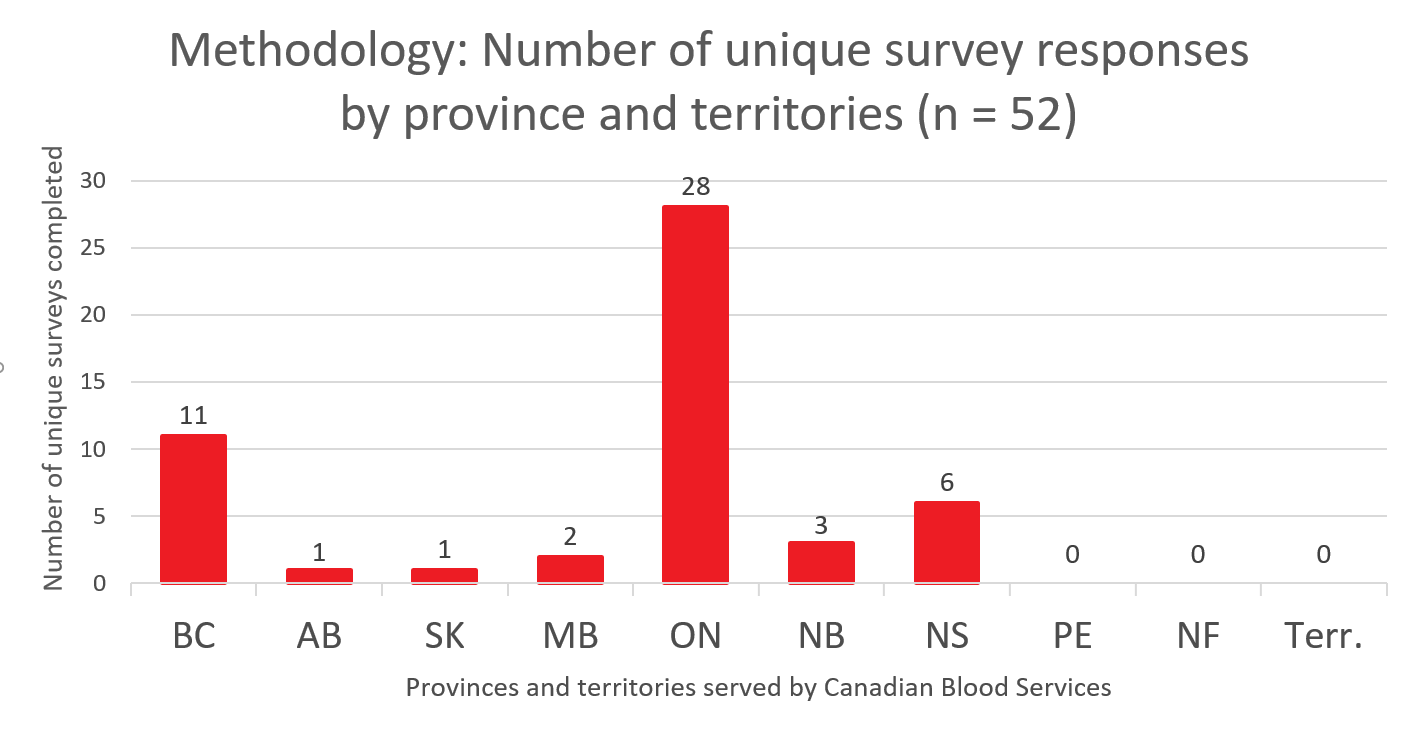
Methodology
This report contains the results of an online survey among Canadian Blood Services hospital transfusion service customers. The survey was administered by Karen Gilmore from Canadian Blood Services Research and Marketing team, using a QuestionPro survey tool.
- 92 hospital contacts were emailed an invitation to participate in the survey. They represent 80% of the platelets transfused by hospitals serviced by Canadian Blood Services.
- In total, 52 unique surveys were completed, for a response rate of 57%.
- The survey was fielded from May 8 to 24, 2019.
Note: Responses provided for “Other” or “Please describe” questions are reproduced exactly as received.
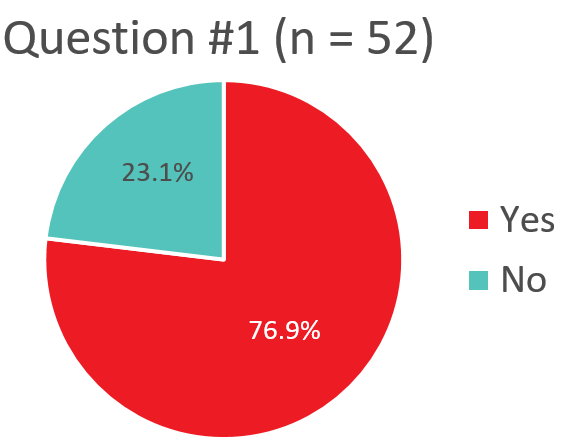
Minimum Threshold
Q1. Does your transfusion service have a minimum threshold for issuing platelets to a stable non-bleeding patient with thrombocytopenia?
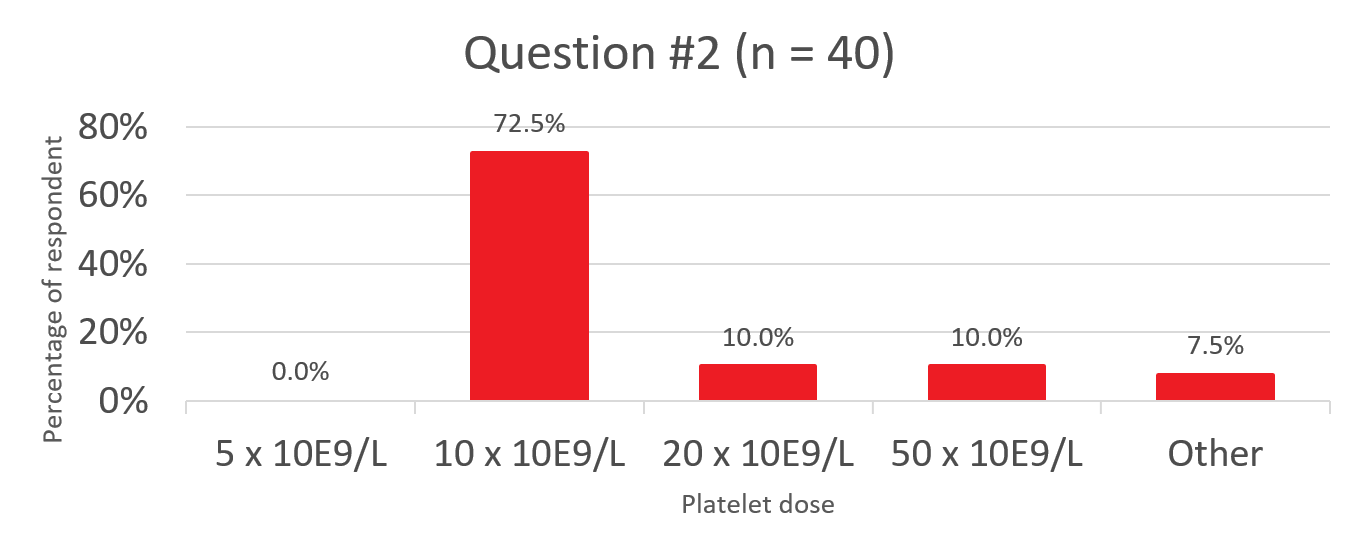
Q2. If yes, what is the transfusion service’s minimum threshold?
Response “Other” – Minimum Threshold
- This depends on the patient’s clinical category and what procedure they are undergoing.
- Plt transfusion is contraindicated in ITP patients.
- 5-20 depending on patient hx.
Platelet Dose for Stable Non-Bleeding Patients
Q3. What dose does your transfusion service generally issue to stable non-bleeding patients who require a prophylactic platelet transfusion?
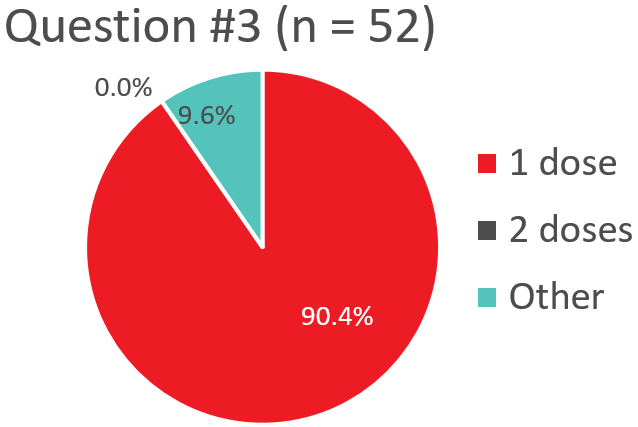
Response “Other" – Platelet Dose for Stable Non-Bleeding Patients
- This depends on the clinical indication and procedure. Generally if 2 or more dose is ordered the order is screen by the TM physician.
- Generally 1 adult dose, dependent on situation.
- Dose is dictated by ordering physician.
- Based on Dr's order.
- None (one response).
When Available, ABO Identical Platelets for Stable Non-Bleeding Patients
Q4. When available, does your transfusion service give ABO identical platelet transfusions to stable non-bleeding patients?
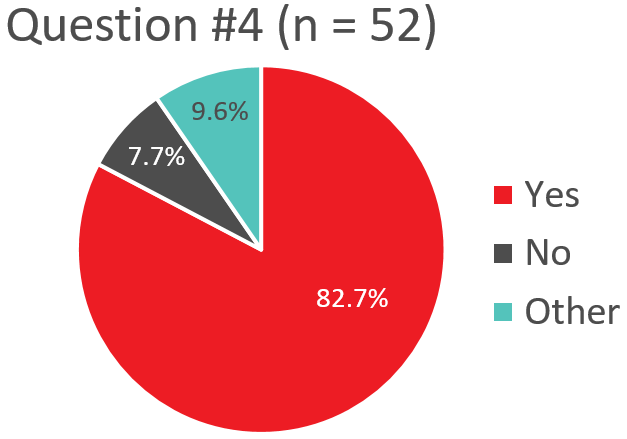
Response “Other” – When Available, ABO Identical Platelets for Stable Non-Bleeding Patients
- We issue according to expiry date.
- Dependent on the outdate.
- We don't transfuse stable non-bleeding pts.
- If inventory management practices allow.
- Whatever expires first.
Use of Rh Immunoglobulin – Patient of Child-Bearing Potential
Q5. Does your transfusion service give female children and women of child-bearing potential who are Rh-negative, Rh immunoglobulin if they are transfused with Rh-positive platelets (unless anti-D is detected)?
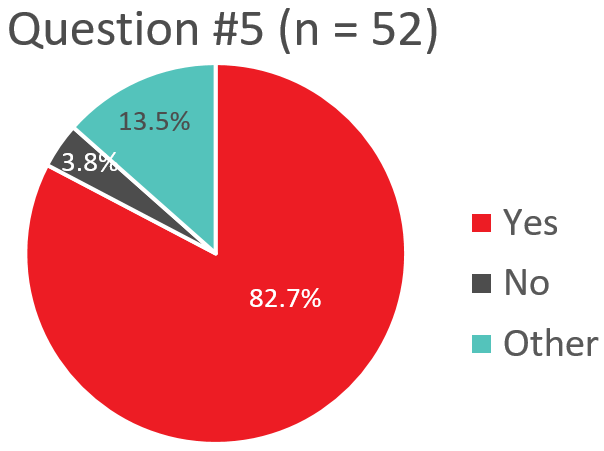
Response “Other” – Use of Rh Immunoglobulin – Patient of Child-Bearing Potential
- TMS Physician notified and recommendation sent to ordering physician, up to physician to request RhIg.
- This is up to the doctor but it is suggested that they do so.
- Only after consult with hematopathologist.
- The Lab will recommend RhIg but ultimately it's the ordering physician's decision
- If order received from ordering doctor, all are notified of option.
- We only give Rh Neg Plts.
- At the discretion of the hematopathologist.
Use of Rh Immunoglobulin – Patient NOT of Child-Bearing Potential
Q6. Does your transfusion service give male patients and women NOT of child-bearing potential who are Rh-negative, Rh immunoglobulin if they are transfused with Rh-positive platelets (unless anti-D is detected)?
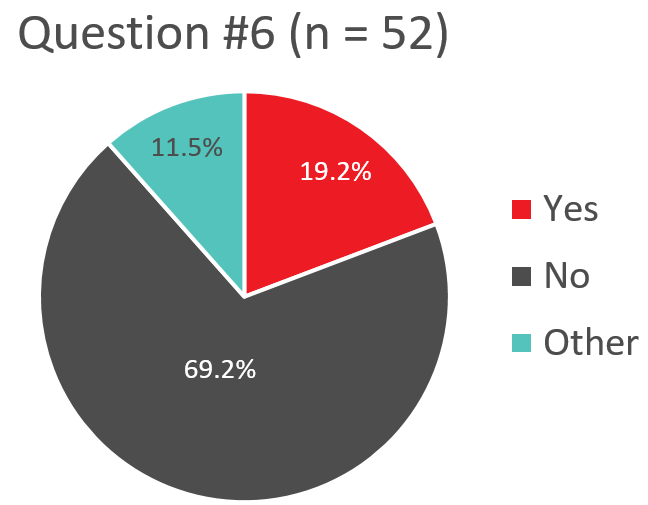
Response “Other – Use of Rh Immunoglobulin – Patient NOT of Child-Bearing Potential
- Hematopathologist decision.
- It is up to the doctor but it is suggested that they do so.
- At the physicians discretion - if a patient that may require ongoing products then yes.
Use of HLA Selected Platelets for Refractory Patients with Confirmed HLA Antibodies
Q7. Does your transfusion service give patients, who are refractory to platelet transfusions, and have confirmed HLA antibodies, HLA selected platelets?
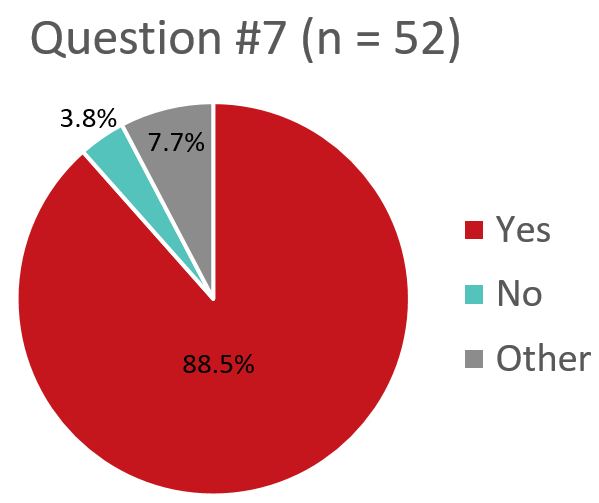
Response “Other” – Use of HLA Selected PLTs for Refractory Patients with Confirmed HLA Antibodies
- If requested can order HLA Plts
- After review and request from pathologist
- We have never had these patients
- We don't manage these patients
Use of HPA Selected Platelets for Refractory Patients with Confirmed HPA Antibodies
Q8. Does your transfusion service give patients, who are refractory to platelet transfusions, and have confirmed HPA antibodies, HPA selected platelets?
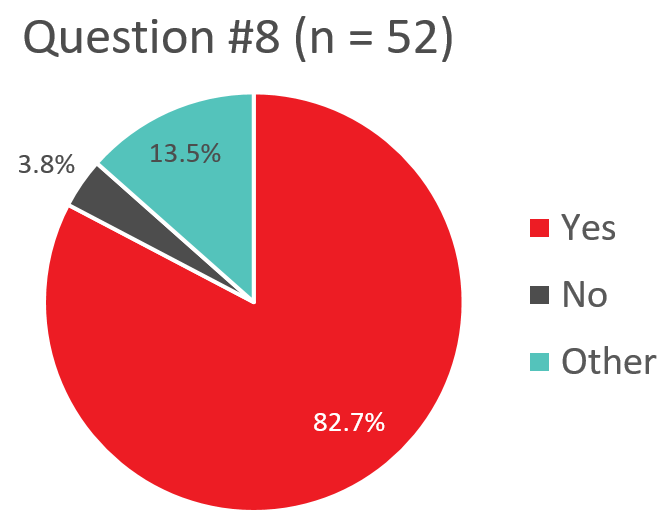
Response “Other” – Use of HPA Selected PLTs for Refractory Patients with Confirmed HPA Antibodies
- Yes, but the would have to be identified to us specifically.
- If necessary, would be investigated with CBS.
- If requested can order HLA plts.
- We have not had this situation to date but we would attempt to do so.
- After review and request from pathologist.
- Not applicable.
- We don't have these patients.
Use of HLA/HPA Selected Platelets for Refractory Patients WITHOUT Confirmed HLA/HPA Antibodies
Q9. Does your transfusion service give patients, who are refractory to platelet transfusions, WITHOUT confirmed HLA/HPA antibodies, HLA/HPA selected platelets?
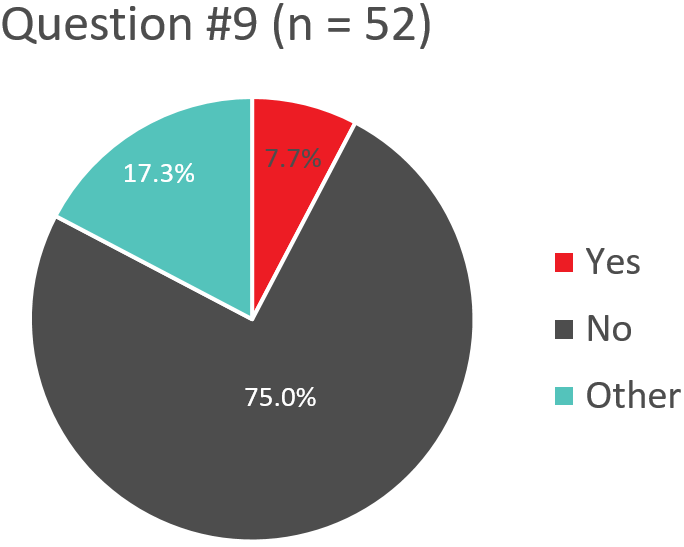
Response “Other” – Use of HLA/HPA Selected Platelets for Refractory Patients WITHOUT Confirmed HLA Antibodies
- Occasionally this may be requested on trial basis.
- Hematopathologist decision.
- Single donor.
- We wouldn't always know.
- If patient has HLA / HPA typing available, we could give HLA matched or HPA matched plts if requested by our medical directors.
- Have never seen any of these patients.
- No for HLA antibodies, Yes if suspected FNAIT or PTP re: HPA selected plts.
- We don't have these patients.
- At the discretion of the hematopathologist.
Use of HLA/HPA Selected Platelets for Non-Refractory Patients
Q10. Does your transfusion service give patients, who are NOT refractory to platelet transfusions, HLA/HPA selected platelets?
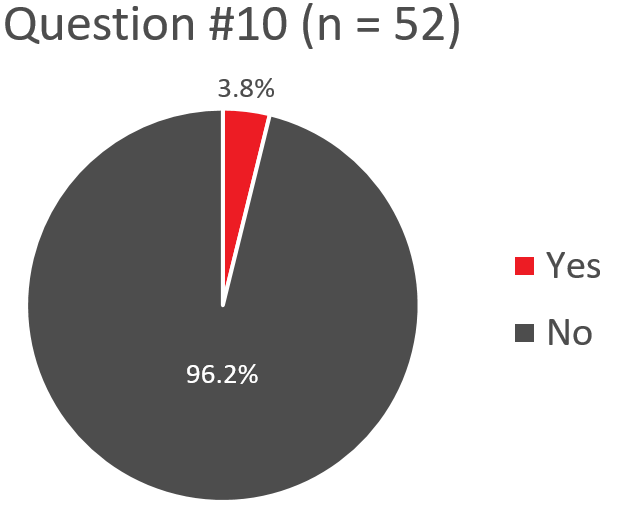
If “Yes”, Describe – Use of HLA/HPA Selected PLTs for Non-Refractory Patients
- Only in circumstances where the HLA platelet will outdate before the HLA patient requires a transfusion. This can happen when treatment for the HLA patient is cancelled or deferred and the Lab does not want to expire the HLA platelet unit; we will transfuse to any patient to avoid discarding the unit.
- Only if intended transfusion is cancelled and product will not be given to recipient; would be issued for general transfusion to avoid expiration.
Pooled and Apheresis Platelets Viewed as Equivalent
Q11. When making issuing decisions, does your transfusion service view pooled and apheresis platelets as equivalent? If no, which platelet type is preferred?
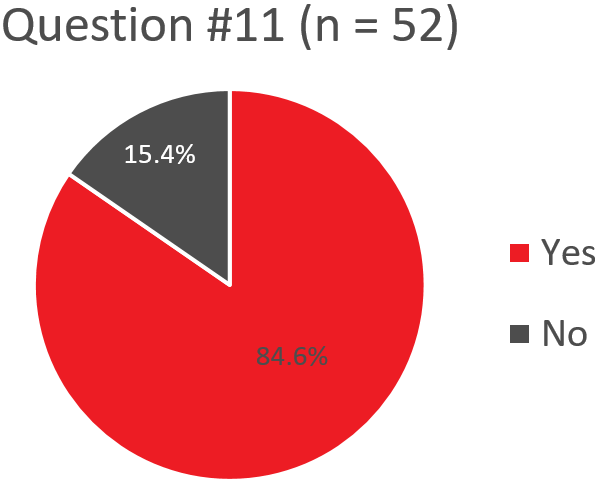
If “No”, Which Platelet Type is Preferred? (Pooled and Apheresis PLTs Viewed as Equivalent)
- Apheresis for BMT.
- Allo transplant patients and neonates - preferred platelets are apheresis. Everyone else receives pooled.
- Approx. 90-95 % of platelets requested at our facility would be apheresis. This product allows us to prepare small volume aliquots for our neonate and pediatric populations. With apheresis platelets as long as we maintain a volume >100ml in the parent bag we can retain the original expiry date.
- Apheresis platelets for neonates to minimize donor exposure.
- Neonatal patients receive apheresis platelets.
- We prefer to use pooled platelets for all of our patients, regardless of bleeding or low platelets. Those patients who seem refractory before HLA/HPA status can be evaluated will also receive pooled platelets.
- Patients that have had previous transfusion reactions to platelets but no HLA testing will try and give apheresis platelets if possible.
- Apheresis is only ordered when requested by physician.
References
1. Endorsement of the ICTMG Platelet Guidelines published by the National Advisory Committee on Blood and Blood products published online (https://nacblood.ca/resources/index.html) on August 6, 2018.
2. Platelet guideline resources on ICTMG website https://www.ictmg.org/platelets-1.
3. Nahirniak S. et al. Guidance on platelet transfusion for patients with hypoproliferative thrombocytopenia. Transfus Med Rev. 2015 Jan;29(1):3-13.