2022 CBR summer students tour the netCAD Blood4Research facility
Our partnership with the Centre for Blood Research (CBR) at the University of British Columbia is helping to train the next generation of researchers in transfusion science. This blog post highlights just some of the achievements in education, training or knowledge mobilization accomplished by CBR trainees.
This post was written by Melody Weng, Tien Do and Christina Pan, all Centre for Blood Research (CBR) at the University of British Columbia summer student alumni (2022). This post originally appeared on the Centre for Blood Research blog in September 2022. Applications for the 2023 Centre for Blood Research Summer Studentship Program are now being accepted! To learn more and apply, visit Undergraduate Summer Research Program - Centre for Blood Research (ubc.ca).
Over the COVID-19 pandemic, the number of active blood donors dropped by 37,000 across the country, leaving Canada at its lowest donor number in a decade. This not only creates a blood shortage crisis for patients in clinics, but also leads to a lack of biomaterials for scientists conducting blood research.
The netCAD Blood4Research Facility helps provide these important biomaterials and blood sources for important research. What exactly is netCAD? Part of the Canadian Blood Services Medical Affairs and Innovation division, it is located at the University of British Columbia (UBC) and produces high quality and prepared blood products for scientists and research institutions.
On August 9th, 2022, our cohort of 12 Centre for Blood Research (CBR) summer students toured the netCAD Blood4Research Facility, to learn more about what they do and how their work benefits scientists and patients alike.
Guided by Le Lam, an experienced coordinator, and Emmanuel Zurbano, a development assistant of over 10 years of lab experience, the facility staff showed us the detailed blood storage process, and how blood components are separated for research purposes. Specifically, they showed us how whole blood – which contains red blood cells, white blood cells, plasma and platelets – is separated into its different components. They also demonstrated how they test for bacterial contaminants in blood, to continue keeping our blood supply safe.
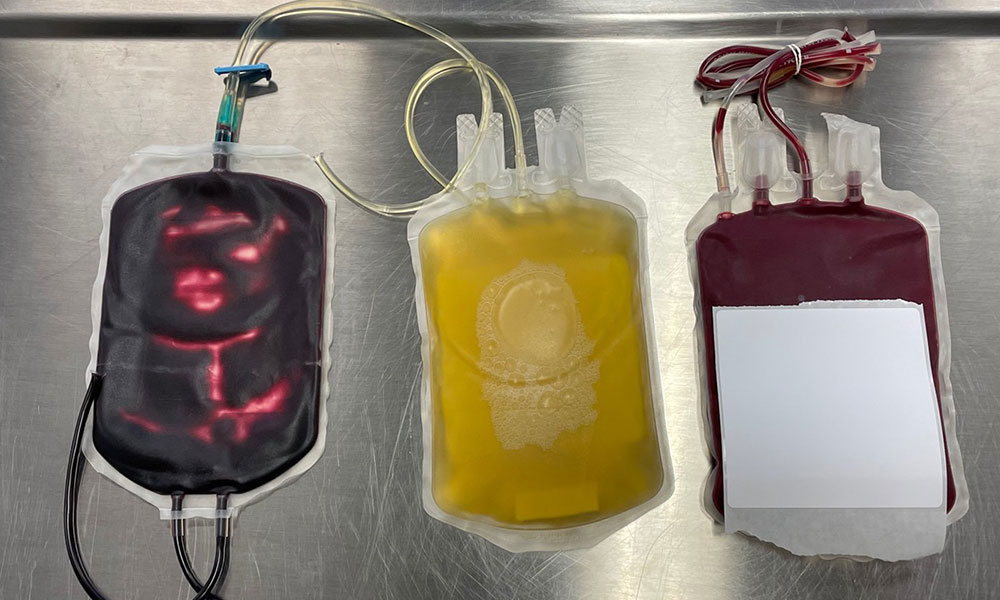
First, the staff placed blood products in a centrifuge. This allowed the blood to separate into layers: heavier hematocrit at the bottom, with platelets (in a buffy coat) on top, and plasma near the top of the blood bag. Using a blood component extractor, the red blood cells, platelet buffy-coat, and plasma are then separated into three different bags.
-
Read more about blood components in Chapter 2 of the Clinical Guide to Transfusion.
Four buffy coat bags from different donors are then connected in a chain, to create what is called a pooled buffy coat. After the pooled buffy coat is centrifuged, the platelets reside in the top layer and residual red blood cells are at the bottom. The platelets are then extracted through a filter to remove white blood cells, and the residual red blood cells are discarded.

Generally, whole blood must be processed into individual components within 1 to 3 days, depending on the components being produced and the temperature during processing. Red blood cells have a shelf-life around 42 days, while platelets can only last for 5 to 7 days. This is why blood separation is crucial: it not only provides us with different blood products for different uses, but also lets us follow storage safety guidelines that are specific to each component.
Next, we learned about bacT testing, a process where platelets are tested for active bacterial contaminants. It’s an important aspect of quality control and ensuring patient safety and is conducted on an as-needed basis for research. Platelets that undergo bacT testing are used in hospital settings, while the other blood products in the netCAD facility are prepared for research purposes.
We also observed another blood donation process, called apheresis, in real time. Unlike whole blood donation, where all components of your blood are collected and later separated, only specific blood components are collected during apheresis thanks to a special instrument used for apheresis, located in the donation clinic!
From this trip, we learned about the intricate processes behind blood donation, how blood is separated into different components, and different ways that you can donate blood products. We also learned how donating blood for research differs from donating blood for clinical use; the first has fewer restrictions on who can be a donor, whereas the latter has stricter requirements because it is more focused on patient safety. This educational trip taught us so much about blood donations for research, and also about the importance of blood donations on a broader scale.
We would like to extend a big thank you to Dr. Peter Schubert, Le Lam, Emmanuel Zurbano, and all the netCAD staff, as well as Dr. Dana Devine, CBR Director, and Dr. Parvin Bolourani, CBR Education Program Manager, for this opportunity!
-
Applications for the 2023 Centre for Blood Research Summer Studentship Program are now being accepted! Learn more and apply before March 10, 2023, using the form available on CBR’s website.

Canadian Blood Services – Driving world-class innovation
Through discovery, development and applied research, Canadian Blood Services drives world-class innovation in blood transfusion, cellular therapy and transplantation—bringing clarity and insight to an increasingly complex healthcare future. Our dedicated research team and extended network of partners engage in exploratory and applied research to create new knowledge, inform and enhance best practices, contribute to the development of new services and technologies, and build capacity through training and collaboration. Find out more about our research impact.
The opinions reflected in this post are those of the author and do not necessarily reflect the opinions of Canadian Blood Services nor do they reflect the views of Health Canada or any other funding agency.